A lack of GP availability is a big part of the reason, health experts say. Photo / Matthew Kay
A Kaitāia woman, who has spent the better part of three years trying to enrol with a general practice nearby, says the system is broken.
Stella Rickit, who is in her sixties, has found accessing
primary care in her hometown nearly impossible as stretched GPs close their books.
An estimated 11,006 Northlanders are not enrolled with a general practice – an overwhelming majority of whom are Māori.
But General Practice Owners Association of Aotearoa New Zealand (GenPro) chairman Dr Tim Malloy said the figure was probably a “gross underestimation”.
A Mahitahi Hauora PHE survey found the main reason behind the “sobering” figures was that GPs are unable to take on new patients.
Rickit and her whānau wait until it is “absolutely necessary” to see a doctor. They make the 350km trip to Auckland to see their current GP, who they have held on to amid the labour shortage.
“When I go to Kaitāia Hospital and I have been for the last three years, I go into Top Health and ask them if there’s any space for me yet to be a patient here,” Rickit said.
/cloudfront-ap-southeast-2.images.arcpublishing.com/nzme/S4HDCC2Y5NFHXANIKJQFRY27BY.jpg)
The answer, as with many GPs in the region, is an apologetic no.
Advertisement
“My concern at the moment is because my husband has had two heart attacks the only people I can count on in reference to a doctor is the one at the hospital, who saved him,” Rickit said.
Data revealed 94.5 per cent of Northland’s 200,660 residents had a GP. The frontrunners were the West Coast and South Canterbury, where 96.5 per cent of each population is enrolled.
Capital and Coast in Wellington and MidCentral in Manawatū were at the other end of the scale. Both districts recorded the highest percentage of the population not enrolled in primary care.
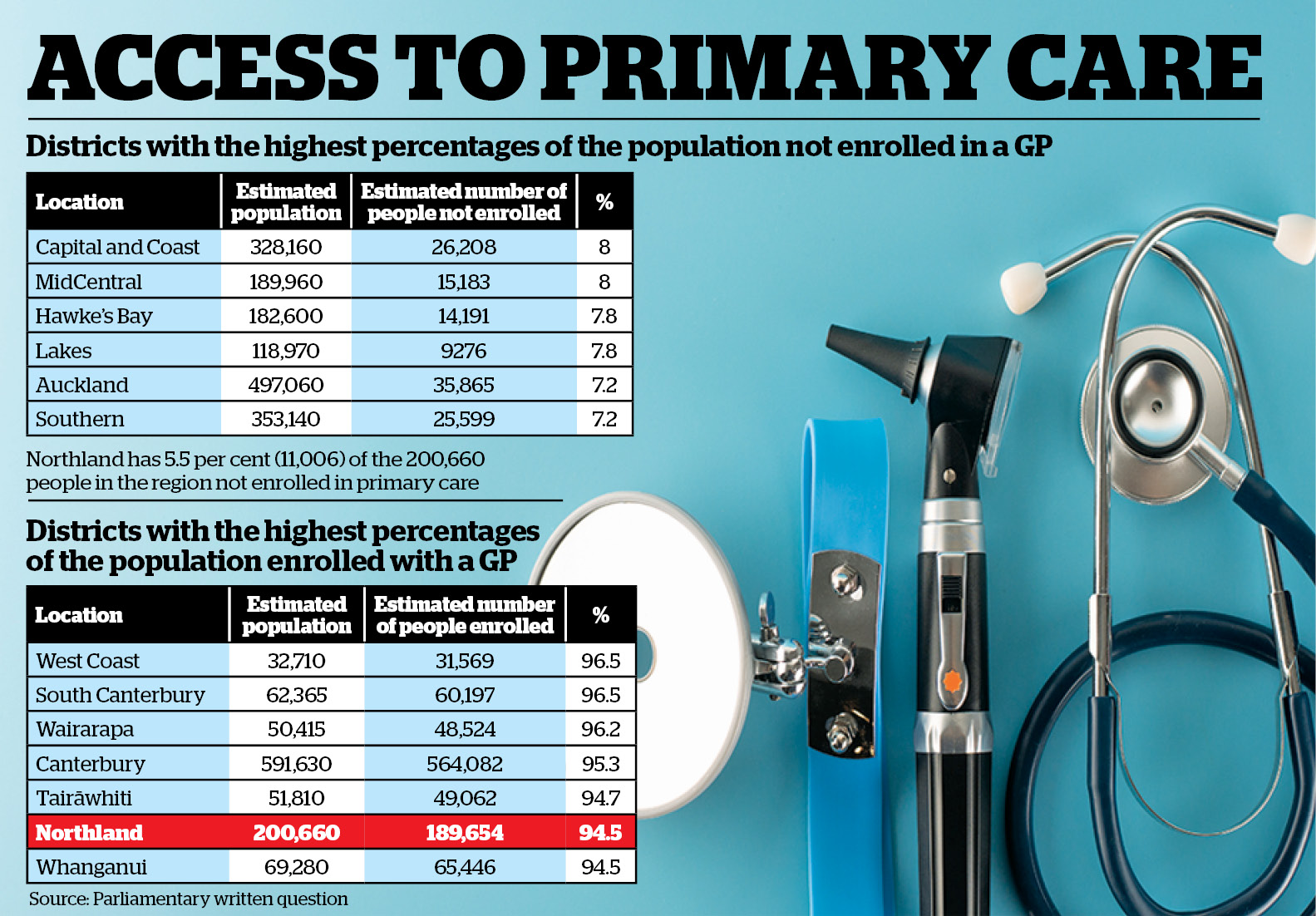
In Northland, 5.5 per cent of its population is without a GP and Ministry of Health figures showed 82 per cent of them are Māori.
Mahitahi Hauora chief executive officer Jensen Webber said the reasons behind the “deeply” concerning inequitable access to GPs were “complex” and “multi-faceted”.
Contributing factors were rural settings, cost barriers – such as transport or time off work to attend consultations; as well as the direct cost of a GP appointment and medications; systemic, cultural and linguistic hurdles, Webber said.
Barriers that disproportionately affect Māori and Pacific Island communities, he continued.
“On a deeper level, inequity of access to GPs is related to inequity in other parts of the health and social sector, as well as in education, economic security, housing, justice, and so on.”
Advertisement
A survey, carried out by the organisation and involving 42 participants – 48 per cent of whom were Māori, revealed the biggest reason people were not enrolled with a practice was because GPs were unable to take on new patients.
Webber said the inability to enrol increased pressure on after-hours services and placed additional demand on practices “already under stress”.
/cloudfront-ap-southeast-2.images.arcpublishing.com/nzme/T33YQTSPBBARPOUGZXU3CIEU24.jpg)
Webber said seven of their 26 practices had their books open. Four of which were in the Far North. However, some were still only enrolling people who lived locally.
Bindi Norwell, group chief executive at ProCare said all of their practices – The Doctors Kerikeri, The Doctors Kamo, The Doctors Tikipunga, and The Doctors Tui – were signing up new patients.
As was four of Comprehensive Care PHO’s 10 Northland practices, according to information provided via the Healthpoint website.
Webber said practices were unable to enrol new patients usually due to systemic reasons, largely beyond their control.
Norwell pointed to the significant workforce shortages.
“We have been advocating for easier access to healthcare professionals for some months now, as have other healthcare providers around the country, including making it easier for healthcare professionals to move and work in New Zealand.”
She said we needed more doctors, nurses, nurse prescribers, nurse practitioners, and medical reception/administrative staff in order to “sustain” the country’s healthcare.
GenPro’s Malloy also cited a lack of funding and increasing workloads as “compromising” GP availability.
“Those of us working in the system want to do it better but we don’t have the people and we don’t have the funding.”
Kelvin Davis, MP for Te Tai Tokerau, said the Government was taking the difficulties accessing a GP seriously.
/cloudfront-ap-southeast-2.images.arcpublishing.com/nzme/6BYMTJLA3K3GUC3AKFHC55MDLE.jpg)
Davis said short-term solutions included GP telehealth options and an arrangement with Kaitāia Hospital for after-hours GP care.
He recognised it wasn’t a long-term solution and said a key part of their strategy was to recruit and train more GPs nationwide.
Davis said the immigration changes around nurses, midwives, and specialist doctors built on “streamlining and funding” the system for international health workers to have their qualifications recognised in New Zealand “making it more attractive for them to move here”.
But Malloy said the inclusion of nurses on the Green List was only going to drive more nurses away from primary care as GPs couldn’t compete with Te Whatu Ora remuneration.
Health Minister Andrew Little said the Government was working to address the issues with “vital” primary care, including building the country’s rural workforce.
“Putting together the first nationwide workforce plan is the Government’s top priority in health. We have reformed the system and I have made this expectation clear to Te Whatu Ora Health New Zealand – it is getting on with the work to do so.
“The health reform has already made it possible for Te Whatu Ora to bring the health system together, establish a single desk for offshore recruitment to manage the arrival of overseas qualified health professionals, as well as run a central recruitment campaign for the health workforce – which wasn’t possible under the old system.”
He spoke of the $4.5 million per year over four years provided by Budget 2019 to help strengthen the rural health workforce, which included a focus on rural GPs.
And the extra funding for additional services GPs were asked to deliver including vaccination and Covid-19 care in the community programmes.
“We also increased funding for GPs for cost pressures by $106 million over the past two years,” he said.
Davis also noted how the Government had launched Te Aka Whai Ora, the Māori Health Authority.
A stand-alone agency, that the MP said would for the first time focus solely on reducing inequity in health outcomes faced by Māori and growing the Māori health workforce.
Webber said Mahitahi Hauora has supported initiatives that increase the proportion of medical graduates entering the primary care workforce in Northland, and the number of skilled mental health professionals and nurses in general practice.
The organisation recently began trialling a virtual clinic hub in two Far North GPs – Te Hiku Hauora and Hauora Hokianga – to help free up time for overstretched GPs.
* Numerators and denominators used in the data are from two different sources (National Enrolment Service vs Stats NZ population projections). Additionally, a small amount of the population still access health services and visit section 88 practices that are not enrolled with a Primary Health Organisation, and therefore, are not counted as enrolled.
What can you do if you don’t have a GP?
Bindi Norwell, group chief executive at ProCare, recommended people ask whether whānau can receive healthcare through their local marae or another wellness provider.
She said telehealth/Healthline, local pharmacies, after-hours/emergency care or mental health providers were also options for health and wellbeing support.
“There are also virtual care options, such as CareHQ, which makes it incredibly easy for people to see a doctor from the comfort of their own home […]”
/cloudfront-ap-southeast-2.images.arcpublishing.com/nzme/HKRPHUYG53V6OVF2TZL7OBOIBU.jpg)
Mahitahi Hauora chief executive officer Jensen Webber recommended people first check Healthpoint or the organisation’s own website to see which practices were taking on new patients.
He said it was sometimes worth contacting people’s first choice practice even if their books are closed because they may be able to fit them in, especially if they live locally or have mobility issues.
But Webber said there was no guarantee.
Anyone who has recently moved to Northland but has a GP elsewhere is encouraged to stick with them until they are able to enrol closer to home.
Webber said people may be able to access primary care as a casual patient at a local GP or Accident & Medical provider, such as White Cross in Whangārei.